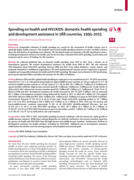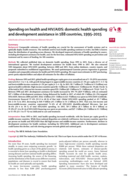General Information
Our Recommendations
New Publications
- Managing transitions from external assistance: cross-national learning about sustaining effective coverage (2024)
- Still rethinking external assistance for health (2024)
- Making development assistance work for Africa: from aid-dependent disease control to the new public health order (2024)
- Understanding China’s shifting priorities and priority-setting processes in development assistance for health (2024)
- Global Economic Prospects (2024)
Filter
174
Featured
Recommendations
1
New Publications
6
Language
Document type
Studies & Reports
138
No document type
26
Strategic & Response Plan
4
Situation Updates
3
Manuals
1
Dashboards/Maps
1
Fact sheets
1
Countries / Regions
Global
44
Africa
4
Lesotho
1
China
1
Nigeria
1
Latin America and the Carribbean
1
Congo, Democratic Republic of
1
West and Central Africa
1
Middle East and North Africa
1
South–East Asia Region
1
Eastern Europe and Central Asia
1
Western and Central Europe
1
Jamaica
1
Japan
1
East and Southern Africa
1
Zambia
1
Indonesia
1
Authors & Publishers
Publication Years
Category
Studies & Reports
3
Health Systems
2
Sexual Violence
1
Health System Strengthening
1
Mental Health
1
NTDs & Others
1
Malaria
1
Toolboxes
General Information & Methodology
100
General Information
72
General Information & Methodology
19
Official Development Assistance
13
Domestic Resource Mobilization
7
Global Health Financing
6
Universal Health Coverage & Primary Health Care
4
Africa
1
Sexual and gender-based violence (SGBV)
1
Orphans & vulnerable children
1
Discrimination & Stigma
1
Sustainable Development Goals
1
Universal Health Coverage UHC and 90-90-90 Strategy
1
Covid-19 & the One Health Approach
1
Children & Mental Health
1
Advocacy & Communication
1
NTDs
1
Strategies & Roadmaps
1
NTDs General
1
Children's Rights
1
General
1
Best Pratice Examples
1
The Abuja declaration identifies that the prevention and control of HIV/AIDS, tuberculosis and related infectious diseases must come with additional financial resources. Therefore, African governments agreed on setting the target of allocating at least 15 per cent of each country’s annual budget ...
Background: Comparable estimates of health spending are crucial for the assessment of health systems and to optimally deploy health resources. The methods used to track health spending continue to evolve, but little is known about the distribution of spending across diseases. We developed improved e...
Background: The last decade has seen a dramatic increase in international and domestic funding for malaria control, coupled with important declines in malaria incidence and mortality in some regions of the world. As the ongoing climate of financial uncertainty places strains on investment in global ...
As a deliverable of the G20 Health and Finance Ministers' Meeting on June 28, 2019, ministers confirmed their commitment to this "G20 Shared Understanding."
Background: Achieving universal health coverage (UHC) requires health financing systems that provide prepaid pooled resources for key health services without placing undue financial stress on households. Understanding current and future trajectories of health financing is vital for progress towards ...
Global growth is projected to slow significantly amid high inflation, tight monetary policy, and more restrictive credit conditions. The possibility of more widespread bank turmoil and tighter monetary policy could result in even weaker global growth and lead to financial dislocations in the most vu...
Objective: There are an estimated 38 million people with HIV (PWH), with significant economic consequences. We aimed to collate global lifetime costs for managing HIV.
Design: We conducted a systematic review (PROSPERO: CRD42020184490) using five databases from 1999 to 2019.
Methods: Studies were ...
Background: Primary health care (PHC) is a driving force for advancing towards universal health coverage (UHC). PHC-oriented health systems bring enormous benefits but require substantial financial investments. Here, we aim to present measures for PHC investments and project the associated resource ...
The accounting framework for health care financing is a key component of A System of Health Accounts 2011, published by OECD, Eurostat and WHO in October 2011.1 The framework makes health accounts more adaptable to rapidly evolving health financing systems, further enhances crosscountry comparabilit...
Background: Sustainable Development Goal (SDG) 3 aims to “ensure healthy lives and promote well-being for all at all ages”. While a substantial effort has been made to quantify progress towards SDG3, less research has focused on tracking spending towards this goal. We used spending estimates to ...
Securing a minimum of financial resources permitting to bring the full range of critical health services to all people constitutes a fundamental human right and an indispensable condition for human dignity. The model outlined here demonstrates that it is within our reach to close the financing gap e...
This paper outlines the background to and design of the Health Financing Progress Matrix (HFPM), WHO’s standardized qualitative approach to assessing country health financing systems. Primarily qualitative in nature, the HFPM assesses a country’s health financing institutions, processes, policie...
The majority of developing countries will fail to achieve their targets for Universal Health Coverage (UHC)1 and the health- and poverty-related Sustainable Development Goals (SDGs) unless they take urgent steps to strengthen their health financing. Just over a decade out from the SDG deadline of 20...
Die Corona-Pandemie zeigt die Bedeutung, die einem umfassenden Engagement der Bundesregierung im Bereich Globale Gesundheit zukommt. Im Standpunkt legen VENRO und das Aktionsbündnis gegen AIDS dar, wie eine adäquate und qualitativ hochwertige globale Gesundheitsfinanzierung aussehen sollte.
According to most recent data, the world economy grew by 3.1 per cent in 2022. To many, the rebound
suggested that a soft landing was possible in 2023, and that the key problems of the year 2022 – rising
prices, supply-chain disruptions and recession risks – have been addressed. As a result, t...
The world has been turned on its head by the coronavirus disease 2019 (COVID-19) pandemic. This has provided a stark wakeup call on the severe under-financing of health systems around the world. It has laid bare the inequalities and limitations in the capacities of countries at all levels of develop...
The 2021 Global monitoring report on financial protection in health shows that before the COVID-19 pandemic, the world was off-track to reduce financial hardship due to health expenditures because trends in catastrophic health spending were going in the wrong direction and the number of people incur...
Dieser Bericht enthält eine neue Strategie für Investitionen in die Gesundheit als Beitrag zur Wirtschaftsentwicklung, vor allem in den ärmsten Ländern der Welt, auf der Grundlage einer neuen globalen Partnerschaft zwischen sich entwickelnden und entwickelten Ländern. Zügiges und mutiges Hande...
Promoting and protecting health is essential to human welfare and sustained economic and social development. This was recognized more than 30 years ago by the Alma-Ata Declaration signatories, who noted that Health for All would contribute
both to a better quality of life and also to global peace a...
Follow up to the so called Abuja Declaration ten years later: In April 2001, heads of state of African Union countries met and pledged to set a target of allocating at least 15% of their annual budget to improve the health sector. At the same time, they urged donor countries to "fulfil the yet to be...